
If you think that you have exhausted the possibilities for naturally staying in another state and have waited long enough, or if the years are coming, it is time to get acquainted with the possibilities offered by modern medicine.
In vitro fertilization procedures are based on improving the couple's natural fertilization capabilities. They are aimed at making contact between eggs and sperm by shortening the path to their connection or bringing them into direct contact. The essence of all IVF procedures is to induce ovulation and deliver the prepared semen to greater or lesser proximity of the ovum in the body (AIH) or outside the woman's body (IVF).
ARTIFICIAL INSEMINATION - AIH OR IUI
Insemination is a simple intervention and lasts from 5-10 minutes and in most cases is completely painless. 1-1.5 ml of previously prepared semen is inserted into the uterus with a special catheter. After insemination, it is recommended that the woman continue to lie down for some time. Two weeks after insemination, it is necessary to do a blood test in order to establish a pregnancy. Insemination is the process of taking the husband's semen (sperm) and its artificial introduction into:
cervical canal - cervical insemination
• transcervical uterine cavity - intrauterine insemination (IUI)
• fallopian tube transcervical - intratubal insemination
Insemination can be one of the types of infertility treatment for couples who have been diagnosed with idiopathic infertility, milder forms of male infertility, and ovulation problems.
Insemination can be reported
• in a spontaneous (natural) cycle at the time of expected ovulation (by determining luteinizing hormone levels)
• with the stimulation of ovulation at the time of expected ovulation (by determining the level of luteinizing hormone) or
• with the stimulation of ovulation at the time of planned ovulation (application of medications that allow us to program the time of ovulation), but always with prior preparation of semen in order to achieve maximum fertilizing potential of the spouse
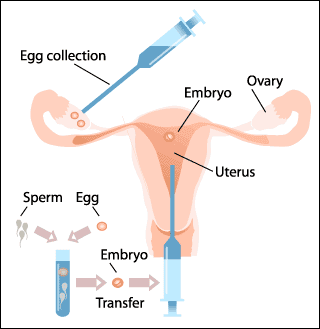

Timing in insemination is very important because insemination is done either immediately before or immediately after ovulation. There are several methods available to doctors to determine the exact date of insemination, such as ultrasound examinations and determination of luteinizing hormone levels.
IUI treatment in the treatment of infertility is recommended a maximum of 3-4 times. If the cause of infertility is the absence of ovulation, insemination can be tried in several cycles, however, most couples who have a problem with pregnancy turn to in vitro fertilization after 3 unsuccessful insemination procedures.
IVF FERTILIZATION - IVF AND ICSI
In vitro fertilization is performed as an infertility therapy only when there is no other simpler way to treat infertility and this method is the crown of infertility treatment and for many couples the only way to parenthood.
We must note that the pregnancy caused by in vitro fertilization is exactly the same as any other pregnancy that occurred in the usual way.
Any complications in such a pregnancy can in no way be attributed to in vitro fertilization.
There are two basic types of IVF procedures - the classic IVF IVF method and ICSI micro fertilization. The decision of which of these two procedures will be applied in the treatment of infertility depending on the number and quality of eggs, as well as the quality of sperm (their number, morphology, and motility). Regardless of which laboratory procedure of merging the egg and sperm is performed, the preparatory phase, which is the procedure of controlled ovarian stimulation, is the same.
Preparatory phase - Stimulation of ovulation
Oocytes develop inside the fluid-filled cavities in the ovaries, called follicles, which enlarge as the egg matures. Controlled ovulation hyperstimulation is a procedure used in in vitro fertilization procedures with the goal of stimulating the ovaries to produce as many eggs as possible, compared to only one as is the case in natural cycles. More eggs, and in connection with that, more embryos, provide the possibility of choosing the highest quality embryos for embryo transfer. The effect of the therapy taken in order to create a larger number of eggs is monitored on ultrasound examinations (folliculometry) and on the basis of the levels of the hormone estradiol. Also, ultrasound monitors the thickness and maturity of the uterine mucosa.
Follicle puncture and oocyte aspiration
In medical terminology, puncture of cavities is referred to as follicle puncture, and egg suction as an aspiration of oocytes. This intervention is performed under general anesthesia, vaginally, under ultrasound control. After the intervention, the biologist immediately examines the submitted material under a microscope and announces the number of obtained eggs.
In vitro fertilization - Laboratory phase - IVF
After collecting the eggs, they are transferred to the laboratory, where they are evaluated and prepared for mixing with sperm. In the case of the classic IVF method, IVF is "offered" a larger number of quality sperm in special conditions. When eggs are inseminated, they are examined approximately 14-18 hours afterward to determine if fertilization has occurred, and 24 hours later to verify that adequate division has occurred.


In vitro fertilization - Laboratory phase - MICROFERTILIZATION - ICSI
In vitro fertilization by intracytoplasmic sperm injection - Microfertilization (ICSI) is an in vitro fertilization procedure used when we want to increase the chances of a couple involved in the procedure, which has a minimal probability of fertilization occurring naturally (classical IVF method). Clinical indications for this in vitro fertilization procedure include:
Male sterility factor
• decreased sperm count
• poor sperm motility
• poor sperm quality
• sperm that lack the ability to penetrate the egg
Immune factor
• idiopathic sterility (of unknown, more precisely, undiscovered cause)
• In previous cycles of IVF, there was no fertilization, or it was significantly reduced, ie. only a very small number of eggs were fertilized.
Under normal circumstances, the egg is surrounded by clusters of cells that must all be removed, and the egg cleaned before the IVF technique is approached. As with the classic IVF method, sperm is obtained from a partner and special laboratory techniques prepare for further procedure. In the most severe cases of the complete absence of sperm in the ejaculate (azoospermia), a testicular aspiration biopsy (TESA) can be performed, ie a real surgical testicular biopsy (TESE). When both sperm and eggs are collected, a process occurs in which the biologist-embryologist injects one sperm into the egg. After this procedure, the egg is examined approximately 14-16 hours afterward to determine if fertilization has occurred, and 24 hours later to verify that adequate division has occurred.
HATCHING
Hatching is a new method that can improve the chances of IVF success in certain situations. By observing the embryos in the laboratory, it was determined that those embryos that are surrounded by a thin natural shell have a higher percentage of implants in the uterine mucosa. This is how the idea of micromanipulation called hatching came about.
On what principles are hatching based?
The embryo that is inserted into the uterus by the usual embryo transfer technique is wrapped in a sheath. In order for it to be implanted in the mucous membrane, the embryo must come out of its shell, that is, it must "hatch" like a bird from an egg. Nature sometimes makes this envelope too thick or firm, so that cells that are in the accelerated division do not have enough energy to break through, and rejection occurs. The solution to this problem is hatching. It thins and pierces the sheath and facilitates the release of the embryo and its subsequent implantation in the mucous membrane. The methods by which this is achieved can be chemical, mechanical, and laser. Lately, the laser has been accepted as the most reliable and is performed in all large biological laboratories. The reliability of the laser in relation to other methods is, above all, the precision of execution, but also the speed.

Hatching is performed immediately before embryo transfer. It is used both on fresh, but also on embryos that have been frozen. Statistics show that less than 1% of quality embryos during this micromanipulation suffer damage that makes them incapable of implantation. However, that is the main reason why hatching is tactically given up in those situations when there is only one embryo. In practice, hatching can be used in all cases of in vitro fertilization. However, experience has shown that this method is especially useful in the following situations:
• later reproductive years, ie in patients older than 37 years
• patients who have elevated basal levels of follicle-stimulating hormone (FSH), which indicates ovarian depletion
• situations where embryonic cells divide more slowly or are fragmented
• in cases where the ova have an evidently thicker and/or firmer sheath (pellucid zone)
• patients who have had several unsuccessful IVF attempts (three or more embryo transfers that did not end in conception)
The results so far show that in all these situations, hatching can increase the chance of pregnancy by 20%.

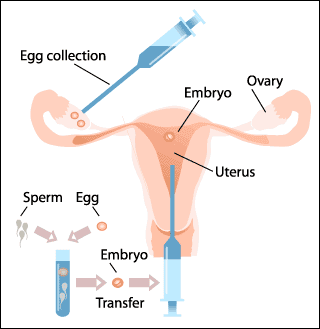
EMBRYO TRANSFER
Embryo transfer, as the end of the in vitro fertilization procedure, can be done as early as thirty hours after the intervention. This means that the return of the embryo takes place from one and a half days to three days after the puncture of the follicles and the aspiration of the eggs.
In certain situations, this period is extended up to five days, until the embryo reaches the "blastocyst" stage. It is important to emphasize that blastocyst culture is not possible for all couples. Not recommended for patients with six or fewer fertilized eggs. The process of inserting the embryo into the uterus does not take long, and it is not painful.
Before the embryo transfer itself, in "Jevremova", patients have the opportunity to see their embryos that will be returned to them. After the embryo transfer, a short rest in our apartments is advised, and after that, the patients are discharged home.
Implant outcome
Fifteen days after the embryo transfer, a test should be done to prove early pregnancy. This sensitive test is called beta-HCG and is done from the blood.






this is one of your best articles, i am a mother of 2 children and now i am trying again to have a third child but failed, i hope to achieve again as a mother, this method has helped all couples, thanks for the wonderful article